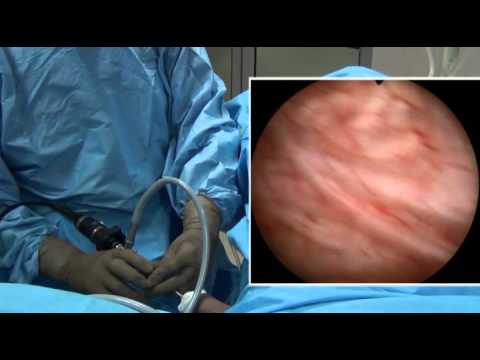
Statistical analysis was built to identify underlying factors that could have influenced anxiety, pain, and/or embarrassment, including gender, age, repeat procedures, and quality of information provided, as well as correlations between anxiety, pain, and embarrassment. The electrodes and rectal catheter were finally removed at the end of the procedure.ĭescriptive results were reported as absolute values (n) and percentages (%) for categorical variables and as mean ± standard deviation (SD) for discrete variables. The urethral catheter was removed and the patient was asked to strain in seated and standing positions. 
To assess VLPP, the bladder was filled a second time until the first sensation of bladder-filling occurred. Cystometrograms, Valsalva leak point pressure (VLPP), pressure flow study with electromyogram (EMG) and post-void residual (PVR) were recorded, tailored to the reason for the test. A room-temperature saline solution was infused at a constant rate of 50 cc/minute with an Aquarius II UDS station (Laborie Medical ULC). The rectal catheter (abdominal pressure 9 Fr, Laborie Medical ULC) was then introduced into the rectum, and the balloon was filled with 3 cc of water. The urethral catheter (dual lumen 7 Fr, Laborie Medical ULC, Mississauga, ON, Canada) was introduced first, after application of a non-anesthetic lubricating gel, and two electrodes (Neotrode ® II, ConMed Corporation, Utica, NY, U.S.) were positioned close to the anal area, at three hours and nine hours, respectively. 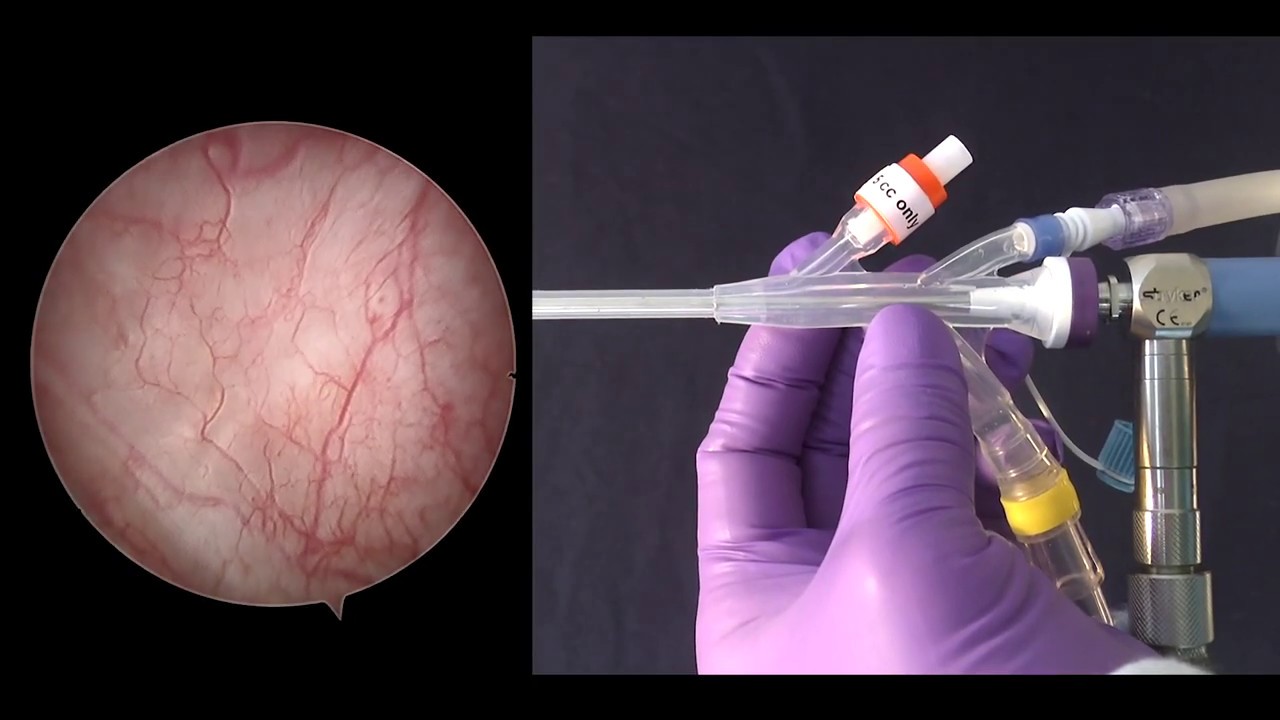
Both men and women were placed in a dorsolithotomy position for the insertion of recording transducers and then seated for the remainder of the study. Free uroflowmetry was followed by clean catheterization (male 16 Fr, female 14 Fr). During their initial consultation, patients received a CUA-produced information pamphlet detailing the procedure. We prospectively assessed anxiety, pain, and embarrassment associated with such procedures and investigated factors that could potentially influence them to find potential ways of improving general tolerance during these examinations.Īll UDSs were performed in an outpatient setting by trained, dedicated nurses. Despite their invasive nature, as recognized by the urological community, comprehensive evaluations of patients’ experience during cystoscopy 1 – 5 and UDS 6 – 9 are scarcely reported in the literature. The procedure aims to diagnose lower urinary tract disorders through continuous measurement of abdominal, bladder, and urethral pressures during the filling and voiding phases. UDS is usually performed in patients complaining of LUTS or presenting neurological diseases suspected to impact the bladder-sphincter system. This procedure allows direct visual examination of the bladder cavity and wall to detect abnormalities, such as diverticula, stones, inflammation, and tumours. Cystoscopy is part of the evaluation process in patients complaining of lower urinary tract symptoms (LUTS) and is undertaken repeatedly in patients being monitored for non-invasive bladder tumours. it will be a short moment of discomfort but wont be painful! and if you keep focussing on the outcome and benefits of having the procedure that will help.Cystoscopy and multichannel urodynamic study (UDS) are essential and valuable diagnostic tools in our daily urological practice. it really really wasnt as bad as i had built it up to be at all. i focussed on breathing in and out slowy and counting, i kept pumping my calms which helps with blood circulation if you're prone to feeling light headed / fainting and i kept repeating in my head, you are fine. my the third appointment i knew i HAD to be ok and couldnt waste another appointment. it took three separate attempts and appointments as i was so scared each time and because i was so worried i kept fainting. I did have a tube put up my urethra for a different procedure a few weeks before which was with no sedation etc. the procedure lasted one minute and was over before i could even realise it had started. im in the Uk so dont know whether that makes a difference. its usually done under general aestephic or sedation however id recently had surgery on my vocal cords so i couldnt. When i went for my cystocopy last year i had an epidural so that i couldnt feel anything from the waist down.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
